The interrelationship of periodontitis and rheumatoid arthritis
A possible mutual effect of treatment is not ascertained. For future studies, it may be valuable to examine subgroups of RA patients, paying more attention to medication and confounders.
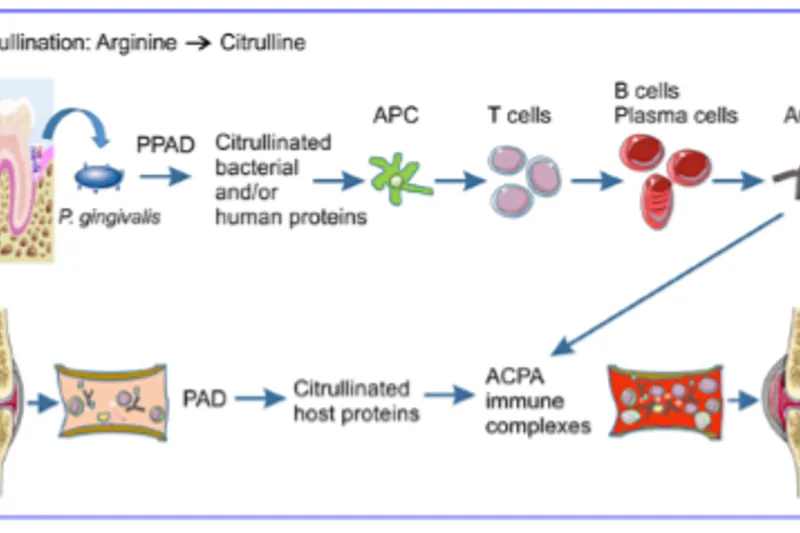
Rheumatoid arthritis (RA) and periodontitis are both common chronic inflammatory diseases and may associate bidirectionally.
The diseases show several similarities in their pathogenesis i.e. inflammatory mediators, cytokines and proteolytic enzymes are largely similar, with a tissue degrading profile in the two conditions. Soft as well as hard tissues are affected.
Both are multifactorial disorders, influenced by a combination of host, lifestyle (smoking), environmental and genetic components, and both have a cyclic nature, fluctuating between chronic and acute periods.
The clinical course of periodontitis in RA patients has been reported as more severe independent of age, gender, ethnicity, or smoking history, and RA patients suffer from increased tooth loss and attachment loss compared with controls.
Periodontitis is a plaque-induced inflammation of the periodontal tissues causing loss of alveolar bone and periodontal attachment.
The periodontal pathogen Porphyromonas gingivalis has been hypothesized to account for a possible link between the diseases through citrullination.
An increased prevalence of periodontitis in RA patients has been shown in several studies. However, the results are conflicting, and a causal relationship has not been revealed.
A possible mutual effect of treatment is not ascertained.
For future studies, it may be valuable to examine subgroups of RA patients, paying more attention to medication and confounders.
Clinical relevance:
Periodontal status is worse in RA patients compared to systemically healthy individuals. RA patients have increased tooth loss and more attachment loss compared to controls. Non-surgical periodontal treatment may reduce clinical symptoms and biomarkers of active RA, but mutual effect of treatment of the diseases is not ascertained. Smoking increases the risk for periodontal disease and RA. It is particularly important that RA patients, who are current smokers, are introduced to a program of regular periodontal follow-up.